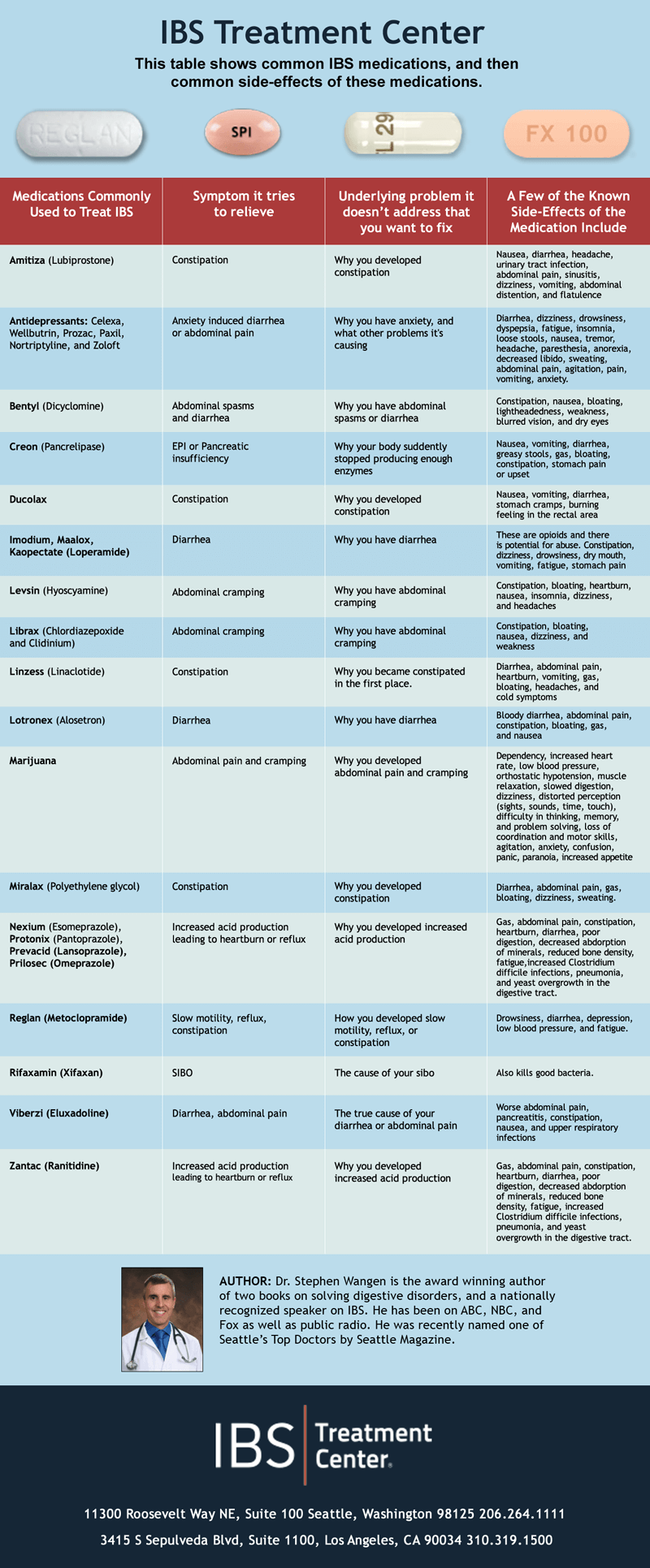
These medications are heavily marketed and highly profitable. But whether or not you should take any of them is a separate matter. They alter the physiology and ultimately the action of the digestive tract, but do they address the underlying causes of IBS, or even claim to cure IBS? And are there any side-effects or warnings that come with these medications? Let’s investigate.
IBS DRUGS ONLY TREAT SYMPTOMS
The typical medical approach for treating IBS involves ruling out other problems and then either doing nothing or trying to suppress symptoms with medications. Many of the patients that come to the IBS Treatment Center have been on numerous medications, none of which has solved their problem. But it’s understandable that people take them because they want relief.
Drugs change how you experience IBS by forcing changes in the biochemistry of your body, sometimes providing temporary relief. Drugs rarely cure IBS. Most medications are designed for temporary use to mitigate the symptoms while the source of the problem is found and addressed. Treatment with these drugs usually does not address the cause of your IBS. Once you stop using the drugs, the symptoms generally return, if you were lucky enough for them to have gone away in the first place.
Research continues on IBS medications, but there will never be a magic pill for curing. IBS is a very broad label. There is no single cause for IBS, and there will never be just one treatment that works for everyone.
IBS is caused by a large numbers of issues that can occur withing the digestive tract. (Click here for more information about IBS causes.) Spending the time to identify and treat the cause of the problem can enable the IBS sufferer to cure their IBS rather than just temporarily treat IBS symptoms like diarrhea, constipation, cramping, etc.
However, more concerning is that the use of these drugs often results in serious side effects and/or negative long-term consequences.
IBS SUPPLEMENTS HAVE THEIR PLACE
Supplements (e.g. things like probiotics, enzymes, and botanical medicine), when of high quality and used in the right person treating the right problem, can have wonderfully positive effects. When not of high quality or used improperly, they can do nothing or even make you feel worse.
At the IBS Treatment Center we often feel the same way about supplements that we do about prescription medications. Supplements are often overused or misused, and patients may use nutritional supplements to mask or suppress their IBS symptoms in the same way that medications can mask or suppress symptoms without addressing the cause of the problem.
Fortunately, supplements generally have less of a downside than medications, though some patients may be spending hundreds of dollars a month on supplements and not realizing any significant benefits. Supplements do have their place, and can have great benefits when used properly.
Our goal is to help patients prioritize what supplements are most needed and eliminate those that are not needed. That includes finding the highest quality products available, using them in the proper dosage, and targeting the right products for the right problems in the right patients.
TYPES OF DRUGS OFTEN USED TO TREAT IBS
Doctors may use several types of drugs to treat the different symptoms of IBS.
They include the following:
- IBS-specific drugs to control the speed with which the bowels move
- Laxatives and other drugs to treat constipation
- Antidiarrheal agents to treat diarrhea
- Antispasmodics to relive the pain from abdominal cramps
- Antidepressants to relieve pain and anxiety associated with IBS
- Narcotic analgesics to relieve pain
- Proton pump inhibitors to block acid production
- Antibiotics
- Enzymes
IBS-SPECIFIC DRUGS
- Reglan (Metoclopramide)
- Reglan is a drug that increases muscle contractions in the upper digestive tract, which will speed up the rate at which the stomach empties into the intestines. It may be used for reflux or for motility disorders.
- It is not intended to be used long term and is not a cure for IBS.
- Most people who take Reglan experience drowsiness. Other side-effects, described in the Journal of Clinical Gastroenterology, include diarrhea, depression, low blood pressure, and fatigue.
- Viberzi (Eluxadoline)
- Viberzi is an opioid and a newer drug for treating diarrhea and abdominal pain. You might recognize the ad for this drug on TV. In spite of the happy ad, it does not cure diarrhea.
- Side-effects include worse abdominal pain, pancreatitis, constipation, nausea, and upper respiratory infections.
LAXATIVES SHOULD ONLY BE USED SPORADICALLY FOR IBS
Fiber supplements and laxatives are often the first things doctors recommend to treat constipation. Laxatives do not cure constipation, and the longer you use them, the more difficult it is to get by without them. Laxatives should only be used very temporarily and sporadically at the most.
If you need laxatives in order to have a bowel movement, then you have IBS and would be better served to find the cause of the problem and eliminate your need for laxatives as soon as possible.
Some drugs used to treat constipation include:
- Linzess (Linaclotide)
- Linzess is a popular, well-advertised medication used in the treatment of constipation. It can cause diarrhea, abdominal pain, heartburn, vomiting, gas, bloating, headaches, and cold symptoms.
- Zelnorm worked similarly and was taken off the market because of the high risk of heart problems and other severe side effects.
- Amitiza (Lubiprostone)
- Amitiza works by increasing fluid in the small intestine to help with the passage of stool.
- It has many side-effects, including nausea, diarrhea, headache, urinary tract infection, abdominal pain, sinusitis, dizziness, vomiting, abdominal distention, and flatulence. It can also cause ischemic colitis, which is life-threatening.
ANTIDIARRHEAL AGENTS DO NOT GET TO THE ROOT CAUSE OF IBS
Many drugs, both over-the-counter and prescription, treat the symptom of diarrhea, but do not get to the root cause of IBS.
- Imodium, Maalox, Kaopectate (Loperamide)
- Imodium, Maalox and Kaopectate are the most commonly-used over-the-counter treatments for diarrhea. They are just as effective, if not more effective, than most of the prescription medications available on the market, but they do not cure diarrhea. They only provide temporary relief of the symptom of diarrhea.
- There can be risks when taking them long term, and many potential side effects. Loperamide is an opioid medication, and therefore there is potential for abuse. We strongly recommend against using it long term.
- Bentyl (Dicyclomine)
- Dicyclomine is an antispasmodic drug that has been around since the 1950s and is used for diarrhea. Potential side effects include constipation, nausea, bloating, lightheadedness, weakness, blurred vision, and dry eyes.
- Lotronex (Alosetron)
- Lotronex may be used by women with diarrhea. It has serious potential side-effects, described in Lancet, including bloody diarrhea, abdominal pain, constipation (in up to 75% of patients), bloating, gas, and nausea.
- Intestinomicina
- This drug is made in El Salvador and the FDA has issued a warning about it saying it can interfere with your body’s ability to make critical red and white blood cells. Taking this drug can lead to serious health problems and even death.
- Questran (Cholestyramine)
- Cholestyramine is a medication that binds bile. It is sometimes used in IBS patients who have problems with their gallbladder and have diarrhea, as described in the American Journal of Gastroenterology. It may help with certain types of diarrhea, but it is not a cure for most types of IBS.
IBS MEDICATIONS FOR CRAMPING
Stomach cramps or abdominal spasms are common symptoms of IBS. They are often in the lower half of the belly, but can be in the the middle or upper abdomen. Some people get worse after meals and feel better after a bowel movement.
- Levsin (Hyoscyamine)
- Hyoscyamine is an antispasmodic drug that has been around since the 1950s. It is used to treat abdominal cramping. Side effects include constipation, bloating, heartburn, nausea, insomnia, dizziness, and headaches, as well as many others.
- Librax (Chlordiazepoxide and Clidinium)
- Librax is a combination of two medications to treat abdominal cramping. One is an antispasmodic and the other is a psychoactive benzodiazepine for treating anxiety and depression.
- Side-effects include constipation, bloating, nausea, dizziness, and weakness. The side-effects can be worse than the original symptoms.
ANTIDEPRESSANTS ARE UNPROVEN FOR CURING IBS
Antidepressants are often prescribed by doctors for IBS. There is a theory that IBS is caused by poor regulation of neurotransmitters in the relationship between the brain and the significant neural network in the gut.
This is an intriguing theory, but it generally doesn’t address the true underlying cause of your IBS, and any poor regulation of neurotransmitters in the gut is not caused by a lack of antidepressant medications. Although some people experience some relief in their IBS while on antidepressants, they do not cure IBS, as noted by Dr. Talley in the American Journal of Gastroenterology.
Brand names of these medications include Celexa, Wellbutrin, Prozac, Paxil, Nortriptyline, and Zoloft, among others. And of course they all also come with many potential side-effects.
PROTON PUMP INHIBITORS COULD MAKE YOUR IBS WORSE
Proton Pump Inhibitors, or PPIs, shut down the production of stomach acid. They are not designed for IBS, but we have seen so many patients who have been put on PPIs by other doctors that we must address them here.
PPIs might make your IBS worse, as described in a study by Dr. Compare. PPIs are also not designed to be used longer than 8 weeks, and they come with a variety of side effects, such as gas, abdominal pain, constipation, heartburn, diarrhea, reduced bone density, increased Clostridium difficile infections, pneumonia, and yeast overgrowth in the digestive tract. Long-term use of the drugs can make it difficult to absorb some nutrients.
Some types of PPIs Include:
- Protonix (Pantoprazole)
- Prevacid (Lansoprazole)
- Prilosec (Omeprazole)
- Nexium (Esomeprazole)
ANTIBIOTICS CAN BE THE CAUSE OF IBS
Some doctors prescribe antibiotics to kill bacteria in the gut, which may be the cause of IBS. This theory has merit for some people with IBS, but broadly using antibiotics, even special antibiotics such as those below, is generally not the best way to treat the IBS. In fact, it’s often why the problem was created in the first place, as described in the American Journal of Gastroenterology.
- Rifaxamin (Xifaxan)
- Rifaxamin is a broad spectrum antibiotic being used to treat Small Intestinal Bacterial Overgrowth (SIBO) which is one potential cause of IBS.
- Rifaxamin is popular in the IBS world lately. It is not necessarily more effective than other antibiotics (see Dr. Bolton’s study), although it’s action is limited to the digestive tract. It can also kill helpful bacteria in your gut.
ENZYMES HAVE MIXED RESULTS FOR IBS
Enzymes may or may not be helpful for treating IBS. One instance where they can be indicated is for pancreatic insufficiency, as described by Dr. Leeds in the journal Gastroenterology. Many are available over-the-counter, and one is by prescription only (and interesting it isn’t any stronger or any better than many others that don’t require a prescription).
- Creon (Pancrelipase)
- Creon is a prescription enzyme.
At the IBS Treatment Center we carry non-prescription enzymes that are exactly like Creon, and some even stronger than Creon, as well as many other types of enzymes.
IBS TREATMENT CENTER FINDS THE ROOT CAUSE OF IBS SYMPTOMS: TO CURE YOUR IBS BY FINDING THE ROOT CAUSE NOT JUST RELIEVING SYMPTOMS

At the IBS Treatment Center, we rarely use any of these medications. Other than antibiotics for bacterial overgrowth, and enzymes for pancreatic insufficiency, the medications listed above have clearly demonstrated their inability to cure IBS. Even worse, almost all these drugs have the potential to make IBS worse.
Our goal is to end IBS symptoms for the long term. To do this, we work to find the true cause of a patient’s problem, not just treat the symptoms. Once we find the underlying cause of the IBS, we can treat it and the symptoms will end, not just be masked by the quick fix of a prescription.
After treatment at our facility, most of our patients are ultimately able to discontinue the use of any previously prescribed medications for their digestion. It is usually a natural transition for a patient to cut back on the meds as they heal and begin to feel better. Without the symptoms, the need to suppress them with medications disappears.
IBS is a complex disorder with a variety of symptoms and causes. There is no one-size-fits-all cause or cure for IBS. Finding your cure requires an experienced medical expert like those at IBS Treatment Center who will spend the time to understand your unique situation and work with you to find the right treatment plan.