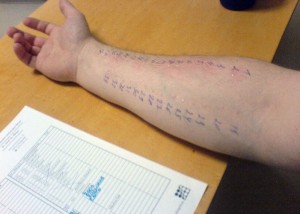
For decades, skin testing has been the standard way to test for allergies.
The potential allergen is injected under or scratched into the skin, and any resulting inflammation (also known as wheal) is measured. The size of the wheal supposedly determines whether or not an allergy is diagnosed. This technique leaves a lot to be desired because we don’t inject food into our skin when we eat, nor do we necessarily get a red bump when we have a food allergy. This is also a subjective test. There is no scientific standard for the amount of swelling required for a positive result.
Equally important, this test can measure only an IgE antibody reaction. And even so, it often is negative, missing elevated IgE levels that are evident with a blood test. The IgG antibody is not tested for at all.
Many people are incorrectly told after skin testing that they do not have a particular food allergy. Others seem to react to everything that is tested.
Skin testing is probably relevant only for life threatening (anaphylactic) types of food allergies, but in these cases the patient often already knows that he or she has the food allergy.
A more accurate way to detect most food allergies is through ELISA (ee-LIE-za) testing of the blood. This test measures the actual amount of both IgE and IgG in the blood. ELISA stands for Enzyme Linked Immunosorbent Assay, a big fancy phrase for a laboratory procedure in which antibodies are detected and measured. This very specialized procedure is performed only by doctors trained in recognizing and treating food allergies. It is run only by specialized labs equipped to handle such sophisticated testing.
QUESTIONS? Feel free to ask in our comments section (below) or contact our office.

Dr. Wangen is the founder and medical director of the IBS Treatment Center, the award winning author of two books, and a nationally recognized speaker on digestive disorders. He has been on ABC, NBC, and Fox as well as public radio, and was named one of Seattle’s Top Doctors by Seattle Magazine.

