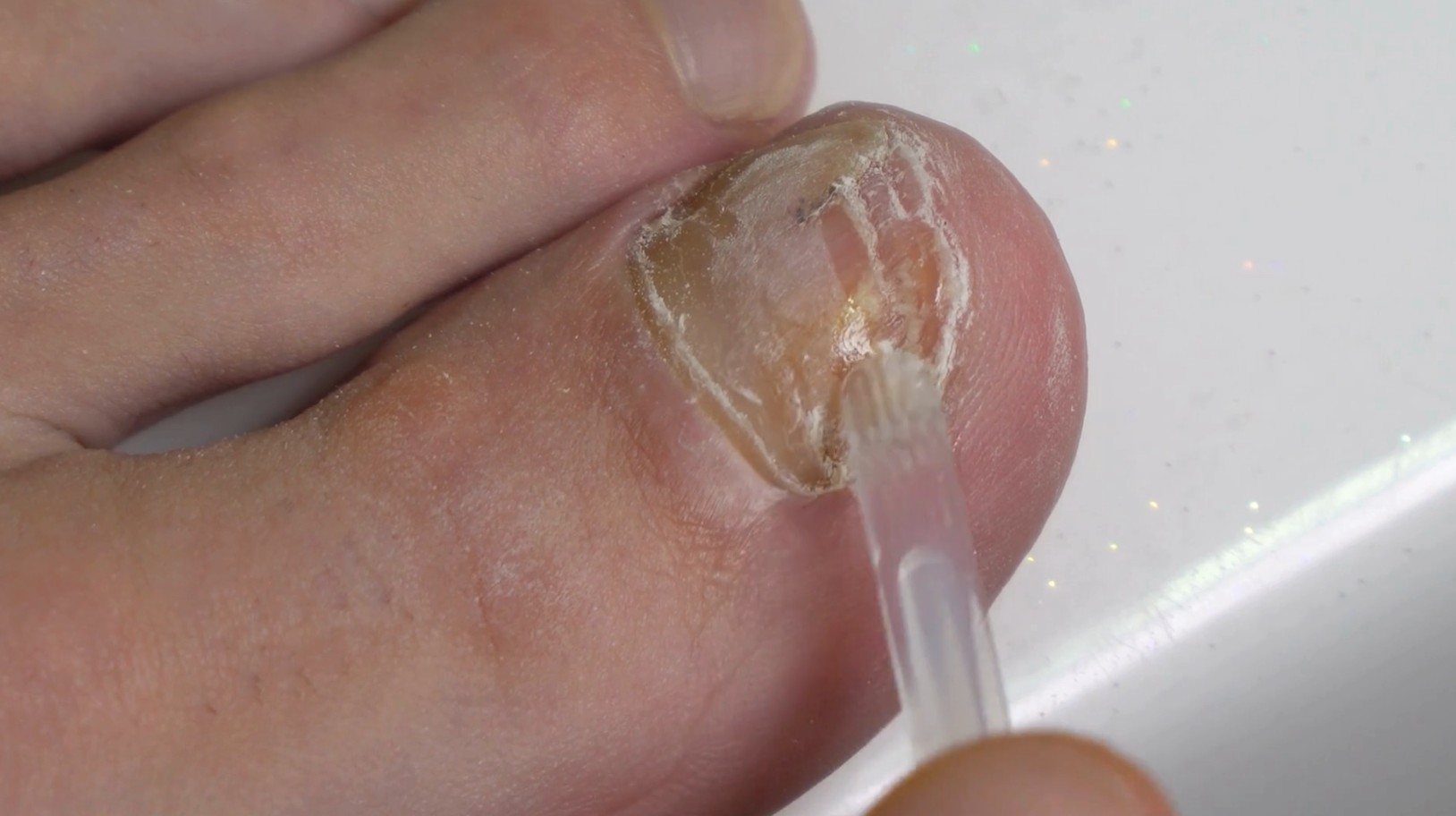
Can gut Candida and toenail fungus actually be connected? At first glance, it sounds unlikely. Candida and toenail fungus are typically caused by different fungi. Could there be a deeper connection through immune function, microbiome health, inflammation, or nutrient absorption?
Read More ->
Dark circles under your eyes? Constant fatigue? Stinky gas? Acne? And nobody can tell you why? I know how frustrating that is—because I lived it myself.
Read More ->
In this video, Dr. Stephen Wangen explains the strange reality behind a digestive health clinic built around helping patients recover — even though that means they often no longer need ongoing care.
Read More ->
If your child is heading back to school next fall and they’re still struggling with digestive problems or abdominal pain, now is the time to deal with it — before school starts again.
Read More ->
If you or your child has ADHD or autism and struggles with gut issues, you’re not imagining it. These problems are incredibly common—and often completely overlooked or misunderstood by most doctors. I’m going to share with you how we approach digestive issues in these patients.
Read More ->
If your child has ongoing stomach pain, lower abdominal pain, constipation, diarrhea, gas, or bloating…And you’re still not getting real answers…There’s a reason—and it’s not something they’ll just grow out of.
Read More ->
Did your doctor actually figure out what’s wrong…Or did they just give your problem a name?Because those are not the same thing.And that difference might be exactly why you’re still not getting better.
Read More ->
Insurance companies focus on codes, costs, and approvals, not patient outcomes. For over 25 years, this digestive health expert has witnessed how the system fails to ask if patients actually improve, leaving many IBS sufferers stuck in an endless cycle. It’s time for change.
Read More ->
Most people assume that if these tests are normal, there’s no inflammation. But that’s not true. These tests only measure specific inflammatory pathways — not all inflammation in the body.
Read More ->
Most doctors don’t guarantee results. In fact, in healthcare you almost never hear the word guarantee. But at the IBS Treatment Center, we actually do.
Read More ->Seattle: 206-264-1111
Los Angeles: 310-319-1500
Our WhatsApp: 206-791-2660
Copyright © 2026 IBS TREATMENT CENTER. All Rights Reserved